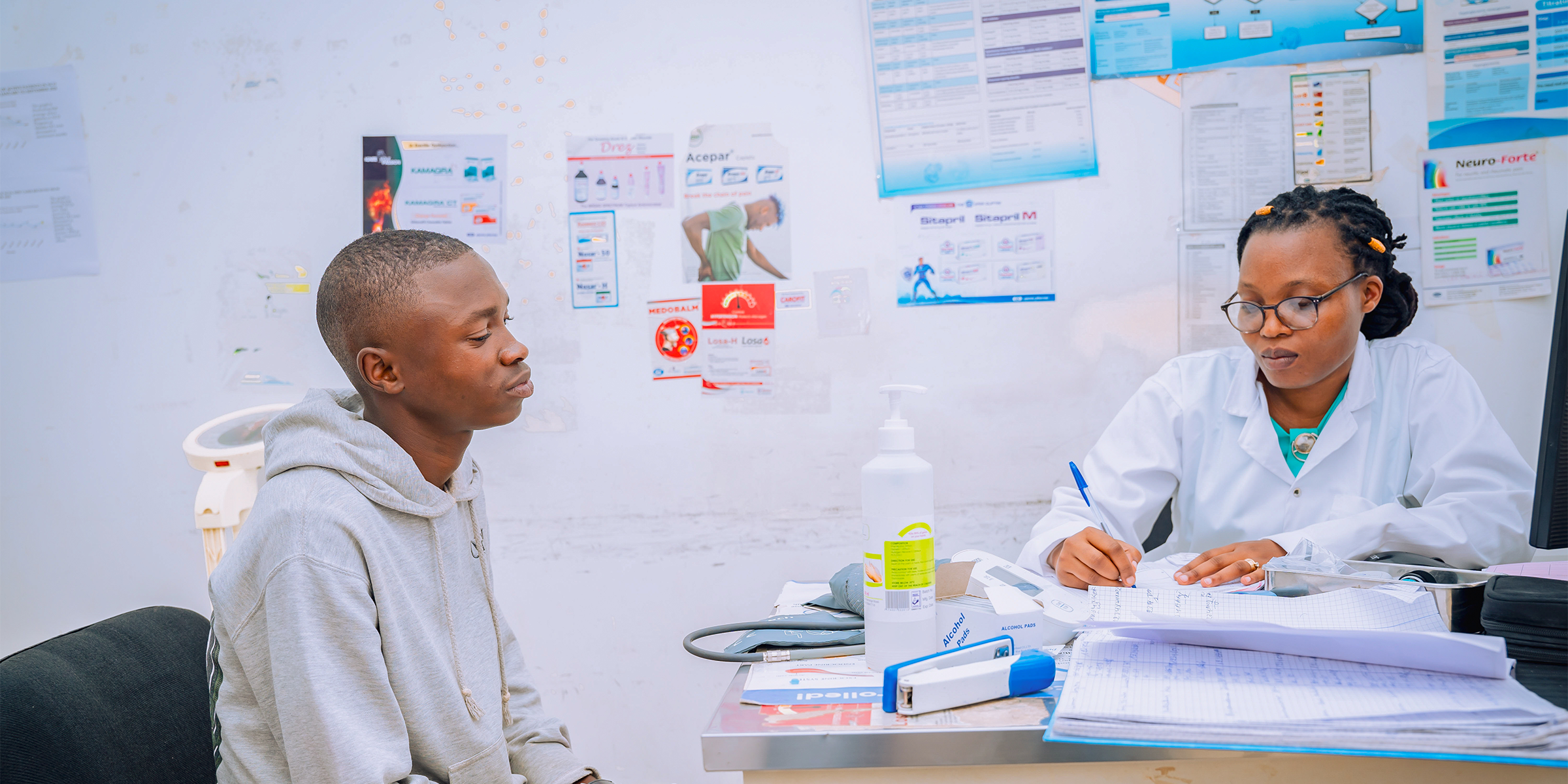
As a clinical instructor at Sister Leonella Consolata Medical College in Nyeri, Kenya, Finlay Matunda spends most of his time interacting with healthcare students in clinical settings. Here he witnesses first-hand the increase in patients with cardiometabolic diseases (CMDs) such as diabetes, hypertension, and heart disease.
According to Finlay, “we are overwhelmed with CMD cases,” and when looking at the theoretical training of his students, he points to an important health workforce skills gap: “You realise they do not have the comprehensive knowledge or comprehensive details on how to manage these patients.”
Finlay’s experience points to a broader issue: noncommunicable diseases (NCDs) are increasingly impacting low- and middle-income countries (LMICs), where 73% of all NCD-related deaths now occur, placing an additional burden on already strained health systems. Kenya, for example, is currently facing a 24% shortage in its health workforce — a figure that could rise to nearly 40% by 2035 if no measures are taken. As a result, the country must reconsider how it can deliver efficient healthcare, including how the workforce can better diagnose, prevent, and treat CMDs through more integrated and effective approaches. The cost of inaction: the rising number of people living with NCDs will not receive the care they need.
Transforming prevention and care through improved education
Recognising this challenge, the Political Declaration of the fourth UN High-Level Meeting on NCDs and Mental Health pledges to increase the size, capacity, and competencies of the health workforce for integrated primary healthcare. An important step will be to strengthen education and introduce CMDs in training programmes and curricula to provide healthcare professionals with the competencies needed to diagnose, treat, and offer guidance on lifestyle and health. This can lead to greater empowerment and self-management and pave the way for collaborative patient relationships, which are crucial for chronic care. As diagnostic and care technologies are evolving rapidly, this is an ideal moment to transform education for integrated, patient-centred CMD prevention and care.
Through its Partnership for Education of Health Professionals (PEP) programme, the Novo Nordisk Foundation seeks to contribute to this transformation. With an aim to reduce inequities in health, PEP strengthens the capacity of educational institutions to deliver quality CMD education for current and future health professionals, starting with India and Kenya.
To date, the PEP partnership in Kenya has spearheaded a comprehensive assessment of training needs at educational institutions, providing valuable insights into current knowledge and skill gaps. The institutions themselves are now in the process of defining the needed improvements. This has already resulted in the development of shorter CMD courses, and the first steps are being taken to integrate CMD into the nationally accredited curriculum.
Need for concerted action
Building a health workforce that can meet evolving population health needs in LMICs is imperative, but it requires concerted action to succeed. Fortunately, in Kenya and across the East Africa region, the need for a future-ready health workforce is gaining recognition at the political level. Initiatives such as Africa CDC’s development of the African Health Workforce Compact and WHO AFRO’s formulation of the Africa Health Workforce Agenda 2035 are significant steps toward harmonising competency-based education standards continent-wide. To integrate CMDs into the implementation, though, there is a clear need to engage the NCD community in the ongoing health workforce dialogues.
A key contributor in this context is the East Africa NCD Alliance (EANCDA), which represents member alliances across eight territories. Through its extensive regional network, EANCDA is well-positioned to advocate for increased investment in the health workforce to support effective NCD responses. Notably, EANCDA played a pivotal role in developing the first East Africa Community regional strategy on NCDs, which secured political commitment to strengthen NCD-related content within health professionals’ education and training.
"The East Africa Community regional NCD strategy has moved us from ad-hoc efforts to a coherent, people-centred response. By embedding NCDs into pre-service and in-service training, we strengthen the health workforce and ensure that every facility — from the smallest health centre to the national referral hospital — is better equipped to prevent, diagnose, and manage NCDs across the region." - Harriet Abeda, NCD Alliance East Africa
By joining forces at the regional and global level, we can help to ensure that health workers in LMICs have the competencies necessary to manage the growing burden of NCDs. We therefore call on governments, professional bodies, and civil society to prioritise sustained investment in NCD-focused training, supportive supervision, and empowerment for the health workforce.